![]()

'MELANOMAGRAPHY' TO IMPROVE SKIN CANCER DIAGNOSIS AND TREATMENT
STUDY SHOWS AGE AND RACE INDICATE RESPONSE TO BLOOD PRESSURE MEDICATION
![]()
'Melanomagraphy' to Improve Skin Cancer Diagnosis and Treatment
![]() he
University of Miami Hospital and Clinics/Sylvester Comprehensive
Cancer Center is among the first centers in the United States,
and the first in Florida, to offer a new procedure to detect
melanomas and other skin cancers early. It uses a noninvasive,
handheld microscope that sees through the surface of the skin
to pigmented areas underneath.
he
University of Miami Hospital and Clinics/Sylvester Comprehensive
Cancer Center is among the first centers in the United States,
and the first in Florida, to offer a new procedure to detect
melanomas and other skin cancers early. It uses a noninvasive,
handheld microscope that sees through the surface of the skin
to pigmented areas underneath.
 Termed
"melanomagraphy," the process uses a video camera built
into a microscope to capture images of the skin's subsurface
that are then transferred to a computer.
Termed
"melanomagraphy," the process uses a video camera built
into a microscope to capture images of the skin's subsurface
that are then transferred to a computer.
"The combination of this digital technology and database information allows us to differentiate between the subtle nuances of benign and questionable cancerous tissue in their early stages," says Robert Johr, M.D., a dermatologist at UM/Sylvester. "Looking at the image on a computer screen, we are able to assess the need for a biopsy."
Until now, most doctors had to rely solely on visual surface observation to detect skin cancer, essentially adopting a "better safe than sorry" philosophy toward excisions and biopsies. The downside to this approach was that nearly half of the costly biopsies and excisions later proved to be unnecessary and often left the patients with unsightly scars.
Early results have been encouraging. Dr. Johr says it spared a 19-month-old toddler from unnecessary, potentially disfiguring surgery. "She (the toddler) was referred to me with a suspicious lesion, but with this new technology I easily and confidently diagnosed a low-risk lesion that presently does not need surgery," says Dr. Johr.
![]()
Patient-Friendly Bladder Cancer Test on Horizon
![]() esearchers
at the School of Medicine are on the brink of finding a painless
and effective method for detecting bladder cancer.
esearchers
at the School of Medicine are on the brink of finding a painless
and effective method for detecting bladder cancer.
"Finding a painless test that would detect bladder cancer and improve the patient's prognosis became a research goal for me," says Vinata Lokeshwar, Ph.D., assistant professor of urology at the School of Medicine.
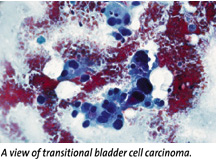 Standard
methods for detecting and monitoring bladder cancer, although
accurate, had been invasive, expensive, and uncomfortable for
patients. Other procedures, such as urine cytology, were easier
to perform, but less accurate.
Standard
methods for detecting and monitoring bladder cancer, although
accurate, had been invasive, expensive, and uncomfortable for
patients. Other procedures, such as urine cytology, were easier
to perform, but less accurate.
Dr. Lokeshwar's research followed a series of hypotheses that originated from molecules that are released in urine by bladder tumors. The HA-HAase test actually comprises two separate urine tests. One looks at the presence of hyaluronic acid (HA), which is significantly elevated in human cancers. The other urine test looks at an enzyme called hyaluronidase (HAase) which promotes the growth of new blood vessels. These vessels supply the nutrients for tumor growth. Consequently, biochemical measurements of HA and HAase were likely to provide a highly accurate method of detection.
To date, Dr. Lokeshwar's HA-HAase test has been 90 percent accurate in detecting the presence of a bladder tumor. The HAase portion of the test also identifies tumor grade, or to what stage the bladder tumor has advanced. Presently, tumor grade can only be identified following biopsy with the patient under anesthesia.
![]()
University Therapists Treat Drug-Abusing Teens at Home
![]() eens
and drugs are a deadly mix. So when teenagers become dependent
on drugs, it often takes a combination of science and a family-treatment
approach to help them regain control over their lives.
eens
and drugs are a deadly mix. So when teenagers become dependent
on drugs, it often takes a combination of science and a family-treatment
approach to help them regain control over their lives.
 The
University's new approach is taking place right in the teens'
homes. Howard Liddle, Ed.D., professor of psychiatry and behavioral
sciences at the School of Medicine, is testing this in-home family
intervention as a method to curtail drug abuse among teenagers.
The
University's new approach is taking place right in the teens'
homes. Howard Liddle, Ed.D., professor of psychiatry and behavioral
sciences at the School of Medicine, is testing this in-home family
intervention as a method to curtail drug abuse among teenagers.
Called Multidimensional Family Therapy, the treatment is offered through the Center for Treatment Research on Adolescent Drug Abuse (CTRADA), a five-year research initiative established at the University with a $6.75 million grant from the National Institute on Drug Abuse. The CTRADA falls under the auspices of the Center for Family Studies in the Department of Psychiatry and Behavioral Sciences.
"Our goal is to test home-based family treatments for drug-abusing adolescents and, in the process, complement their treatment with other services such as tutoring and job and academic skill development," says Dr. Liddle, also deputy director of the Center for Family Studies.
This large-scale project is testing the effectiveness of in-home family therapies as an alternative to in-patient or residential treatment. The program also encourages positive involvement among all members of the teen's life-friends, parents, and teachers. Researchers expect that this therapy will help parents and teens communicate better with each other and learn to negotiate solutions to problems that have caused conflict in the past.
![]()
Insulin Inhalers Could Replace Daily Injections
![]() aking
insulin without the use of needles may be the wave of the future
for many insulin-dependent diabetics.
aking
insulin without the use of needles may be the wave of the future
for many insulin-dependent diabetics.
"Inhaled insulin," delivered through a flashlight-sized, aerosol inhaler similar to those used to deliver the many asthma drugs on the market today, has proven to control blood sugar levels as well as the several daily injections some diabetics have endured for decades.
Jay S. Skyler, M.D., professor of medicine, pediatrics, and psychology, has led two phases of inhaled insulin research and presented results of the initial trial at the American Diabetes Association's Annual Scientific Sessions in 1998.
According to Dr. Skyler, the second phase was the last to be completed before petitioning the FDA to make the drug available to the general public. "In the first phase, we looked at inhaled insulin and its efficacy as a delivery system," says Dr. Skyler. "We've spent the last six months nailing down the specifics of dosage."
Inhaled insulin should to be available for widespread use by late 2000.
![]()
 Adjunct Pharmacologist Furchgott Shares
Nobel Prize
Adjunct Pharmacologist Furchgott Shares
Nobel Prize
![]() obert
F. Furchgott, Ph.D., adjunct professor of molecular and cellular
pharmacology at the School of Medicine, has won a share of the
Nobel Prize for Medicine.
obert
F. Furchgott, Ph.D., adjunct professor of molecular and cellular
pharmacology at the School of Medicine, has won a share of the
Nobel Prize for Medicine.
Dr. Furchgott and two colleagues discovered that nitric oxide acts as a signal for the cardiovascular system, the effects of which range from treating heart disease and shock to the development of the anti-impotence drug, Viagra.
Dr. Furchgott, whose home base is the State University of New York at Brooklyn, has spent the past ten winters at the University of Miami conducting his pioneering research, collaborating with University researchers, teaching seminars, and interacting with students.
In 1980, Dr. Furchgott discovered a substance in the endothelium-a layer of cells lining the innermost surface of blood vessel-that causes the underlying smooth muscle to relax. He called the substance endothelium-derived relaxing factor, or ERDF. This discovery provided the first indication of the crucial role that the endothelium plays in cardiovascular health and disease. ERDF later was found to be nitric oxide.
Dr. Furchgott shares the prize with colleagues from the University of Texas and UCLA.
![]()
School of Medicine Sets Research Priorities
![]() o
better identify its future research priorities, the School of
Medicine is developing six research umbrellas under which scientists'
related investigative activities can be grouped. This strategic
planning process will help the school assign precious resources
and set future fundraising goals.
o
better identify its future research priorities, the School of
Medicine is developing six research umbrellas under which scientists'
related investigative activities can be grouped. This strategic
planning process will help the school assign precious resources
and set future fundraising goals.
"It is not possible for our institution to cover all aspects of medical research," says Senior Vice President for Medical Affairs John G. Clarkson, M.D., dean of the School of Medicine and chair of its research task force. "We must focus on current strengths and identify other areas where we can develop centers of excellence."
 For
the past year, some of the school's most brilliant scientific
minds have been looking at the strengths, weaknesses, needs,
and other issues facing the six areas. The umbrellas include
both existing and new programs, including the following:
For
the past year, some of the school's most brilliant scientific
minds have been looking at the strengths, weaknesses, needs,
and other issues facing the six areas. The umbrellas include
both existing and new programs, including the following:
- Cell growth and development Cancer research is the primary component of this area. The University of Miami Hospital and Clinics/Sylvester Comprehensive Cancer Center has a strong patient base and is currently beefing up its research enterprise. The school's growing wound healing research program also strengthens this area.
- Behavior The school's fastest growing area for the past decade includes programs in adult development and aging, behavioral medicine, child and family studies, HIV/AIDS, and substance abuse.
- Human immunology This area includes a common thread through disease groups as diverse as cancer, diabetes, HIV/AIDS, and other infectious diseases, and organ and cellular transplantation.
- Neurosciences With a quarter of the school's National Institutes of Health grant support, this is the school's greatest strength. In addition to spinal cord injury, stroke, trauma, vision, hearing, and neuro-degenerative disease research, the school has a strong interdisciplinary neuroscience graduate education program.
- Vascular biology This area relates to most pathological processes of the organ systems, including heart disease, stroke, kidney disease, pulmonary hypertension, cancer, and some forms of organ transplantation.
- Health services research A relatively new field in medical research, focusing on outcomes research, this area seeks to find the most effective medical treatments for various diseases. Health services research ultimately will help decision-makers design and operate a more cost-efficient health care system.
Last year, the school conducted more than $112 million in biomedical research. The strategic plan is designed to help the School of Medicine compete more effectively for funding from the National Institutes of Health and other funding agencies, as well as from industry officials and philanthropists.
Business plans are being developed which will consider specific strengths, weaknesses, opportunities, and threats in each area, while projecting one-, three-, five-, and seven-year needs. Funding plans will stem from the business plans. Future issues of University of Miami Medicine will focus on each research umbrella and chart its development.
![]()
Faculty Practice Adopts UMCare Brand Name
![]() he
University of Miami Medical Group has chosen a new brand name
for its clinical service-UMCare-which soon will be seen in advertisements,
signage, and other promotional materials.
he
University of Miami Medical Group has chosen a new brand name
for its clinical service-UMCare-which soon will be seen in advertisements,
signage, and other promotional materials.
"UMCare will be a rallying point for all of our physicians, nurses, therapists, and other professionals who provide care," says Brian Craythorne, M.D., senior vice president for medical affairs and managing director of the faculty practice. "We've needed a strong, consistent, defining identity that will help distinguish us in a very competitive marketplace."
While the physicians' practice will take the name UMCare, the school's existing centers will retain their names. The Bascom Palmer Eye Institute and the Sylvester Comprehensive Cancer Center, for example, have strong identities and will market themselves as components of UMCare.
The new identity will be launched officially in the fall of 1999.
![]()
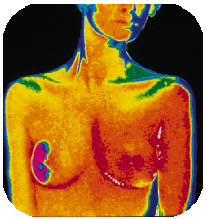
Mapping Breast Cancer's Path in the Body
![]() reast
cancer surgeons at the University of Miami Hospital and Clinics/Sylvester
Comprehensive Cancer Center have identified a technique that
could reduce unneeded lymph node surgeries in breast cancer patients
by nearly 80 percent.
reast
cancer surgeons at the University of Miami Hospital and Clinics/Sylvester
Comprehensive Cancer Center have identified a technique that
could reduce unneeded lymph node surgeries in breast cancer patients
by nearly 80 percent.
 "In
early-stage breast cancer cases, the sentinel node, or the initial
set of lymph nodes under the arm, is typically removed because,
if the cancer spreads, it usually hits these nodes first,"
says Frederick Moffat, M.D., a surgical oncologist at UM/Sylvester
and a co-principal investigator in the study. "Doctors had
found that removal was unnecessary in 70 to 80 percent of cases,
yet there was no way of knowing until the nodes were removed
and tested."
"In
early-stage breast cancer cases, the sentinel node, or the initial
set of lymph nodes under the arm, is typically removed because,
if the cancer spreads, it usually hits these nodes first,"
says Frederick Moffat, M.D., a surgical oncologist at UM/Sylvester
and a co-principal investigator in the study. "Doctors had
found that removal was unnecessary in 70 to 80 percent of cases,
yet there was no way of knowing until the nodes were removed
and tested."
Since lymph node removal is expensive and often followed by postoperative complications, doctors had been searching for an alternate procedure to assess whether the cancer had in fact spread to the lymph nodes.
In an 11-center national study of 443 patients, Dr. Moffat and his colleagues used a mapping technique that uses an injected radioactive dye that interacts with the cancerous cells that may be spreading from the initial tumor. Injected several hours prior to surgery, then identified with a gamma counter, this dye provides surgeons with a road map of "hot spots" representing underlying cancerous sentinel nodes, marking the cancer's path and revealing how many lymph nodes, if any, need to be removed.
"The mapping technique had a 97 percent success rate in identifying those patients that truly had cancer spreading to the lymph nodes," says Dr. Moffat. "This is particularly important, not only because we are able to spare patients from painful surgery and recovery, but the status of the lymph nodes in a patient with early-stage breast cancer is our most powerful variable in identifying survival and possible recurrence," he says.
The results of the breast cancer study were published in The New England Journal of Medicine.
For more information on the mapping technique, contact UM/Sylvester at 305-545-1111.
![]()
Study Shows Age and Race Indicate Response to Blood Pressure Medication
![]() he
factors of age and race are good indicators of what blood pressure
medication is best for you.
he
factors of age and race are good indicators of what blood pressure
medication is best for you.
 That's
what hypertension specialists from the School of Medicine have
identified in a study published with the Miami Veterans Affairs
Medical Center and the Department of Veterans Affairs Cooperative
Subgroup on Antihypertensive Agents.
That's
what hypertension specialists from the School of Medicine have
identified in a study published with the Miami Veterans Affairs
Medical Center and the Department of Veterans Affairs Cooperative
Subgroup on Antihypertensive Agents.
Researchers compared plasma renin lab testing (plasma renin is an enzyme involved in the regulation of blood pressure) to using a patient's age and race to select the most responsive blood pressure medication.
"Patients respond differently to blood pressure medication based solely on their age and race-different medications are recommended for younger black men, younger white men, older black men, and older white men," says Richard A. Preston, M.D., associate professor of medicine and lead author on the study. "Using this age-race indicator is not only cost-free, but effortless to the patients." (Plasma renin profiling requires patients to undergo lab testing and a 24-hour urine collection sample.)
Co-authored with Barry J. Materson, M.D., professor of medicine, the results of the study were published in The Journal of the American Medical Association.
![]()
![]()
![]()
![]()