The catastrophic earthquake that ravaged the already fragile Haitian capital of Port-au-Prince on January 12 unleashed an unprecedented humanitarian crisis. The devastation was beyond belief, the suffering horrific. Yet the brave people of Haiti were stoic in rescuing their neighbors and friends, the injured and the homeless, triggering an impassioned humanitarian response from around the world that showed Haiti will never be forgotten, nor forsaken.
Led by Barth Green, M.D., chairman of neurological surgery, an army of our doctors, nurses, and staff would be joined by more than 2,700 medical volunteers from the U.S. and beyond, who staffed the most advanced ground zero hospital in the hemisphere’s poorest nation. In a 25,000-square-foot tent facility erected by a team led by Ron Bogue, assistant vice president for facilities and services, we collectively treated close to 30,000 patients, saving countless lives.
I will never forget the night of January 17, when I landed in Port-au-Prince with one of the first hospital shifts. I was joining our team in Haiti to assess the needs and develop with Barth and other UM leaders a strategy for our long-term relief effort. We were immediately immersed in the formidable rescue, caring for hundreds of injured Haitians who were brought to two cargo tents at the non-functioning airport. In an improvised emergency room, our volunteers performed life-saving procedures on patients whose survival hung by a thread. One young man, Junior Clermond, had a crushed leg and was suffering from rhabdomyolysis. In need of dialysis, which was unavailable, the 19-year-old would surely die. With a plastic carpet, we lifted him onto a plane bound for Miami, where he would receive the treatment that saved his life. As he bravely awaited takeoff, he asked me to speak to his mother, who stayed quietly behind.
 |
The dead, dying, and injured were everywhere. I was, to say the least, overwhelmed, as probably everybody else was. But our teams in Port-au-Prince and Miami worked beautifully together to ensure that volunteers, supplies, and other necessary equipment were dispatched like clockwork.
The next morning, a 13-year-old girl needed plastic surgery for her chest. A falling rock had sheared off her flesh and rib. Enrique “Iky” Ginzburg, M.D., professor of surgery, and I took her to the Israeli Army Field Hospital, the only one with a plastic surgery service. Our driver, his hand locked on the horn, drove the makeshift ambulance at 70 miles per hour through roads jammed with people, bicycles, cars, and trucks, all trying to navigate a world of chaos. Somehow we made it with our young patient, who said not one word nor shed a single tear. Our Israeli friends traded her for a patient for whom only we were prepared to care. I could not help but think that if all our fellow humans would always interact in such a kind, collaborative way, the world would be a better place.
 |
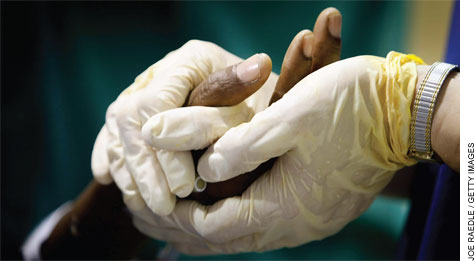
| Haitian patient Junior Clermond, center, is assisted by a care team including, from left, Dean Pascal J. Goldschmidt, M.D., Enrique Ginzburg, M.D., professor of surgery, and Daniel Pust, M.D., critical care fellow. |
The Miller School relief effort was extraordinary—from top-notch trauma care by the UM/Jackson team of doctors and nurses to the can-do spirit of our orthopaedic surgeons, anesthesiologists, pediatricians, OB/GYNs, epidemiologists, dermatologists, neurologists, ophthalmologists, and physical therapists, who pitched in every way they could, even taking orphans under their wing; from the expansion of our pre-earthquake programs in comprehensive health care for underserved Haitians to the introduction of telemedicine to transmit real-time images of patients for consultations with experts in Miami; from the prosthetic limbs and physical therapy provided to hundreds of new amputees to the distribution of hundreds of eyeglasses and the establishment of an eyeglass library by the Bascom Palmer Eye Institute.
Of course, little of this would have been possible without the caring generosity of Stuart Miller, Alonzo Mourning, Eric Feder, Carnival Cruise Lines, the students of Ransom Everglades School, and all the others who collectively contributed $5.8 million, donated their planes, pilots, personnel, and considerable energy or pharmaceuticals, supplies, and equipment to help us help our neighbors in their greatest time of need.
The UM Global Institute for Community Health and Development has since passed the baton for day-to-day operations of our field hospital to our partner in Haiti, Project Medishare, which is leading the effort to establish a desperately needed national trauma, critical care, and rehabilitation network in the nation, as well as the educational components to support them.
Slowly but surely, Haiti is rebuilding. Tim Dixon, Ph.D., professor of marine geology and geophysics, whose team helped us understand the risks as we sent people to Haiti, and other University specialists later convened world experts committed to reconstructing the nation with earthquake-resistant buildings.
As we look back, we have learned so much from this tragedy. Our psychology/ psychiatry teams are helping Haitians surmount their loss and pain in reconstructing a nation that, as it did when it became the first independent state in Latin America, can look toward a future of hope and promise. I am so proud to review what the Miller School did as a team, thanks in no small measure to the wonderful relationship Barth has with the Haitian people, who did all they could to facilitate our mission. To those who delivered God’s work in Haiti, to those who stayed here to support the relief effort and continue to serve our patients, advance our research, and provide outstanding education, and to those who opened their hearts and their checkbooks, I thank you from the bottom of my heart. There is no better team in the world.
|
 |
 |