 |
 |
|
 |
 hrough a labyrinth of hallways with bright blue walls, where balloons
and kites dot the landscape and hushed sounds guard the sleep of sick
children, a thin white needle gauges the first breaths of a new life.
A plastic tube snakes toward a mouth smaller than a rosebud, allowing
a machine to assist tiny pink lungs that were not yet ready to leave a
mother’s womb.
hrough a labyrinth of hallways with bright blue walls, where balloons
and kites dot the landscape and hushed sounds guard the sleep of sick
children, a thin white needle gauges the first breaths of a new life.
A plastic tube snakes toward a mouth smaller than a rosebud, allowing
a machine to assist tiny pink lungs that were not yet ready to leave a
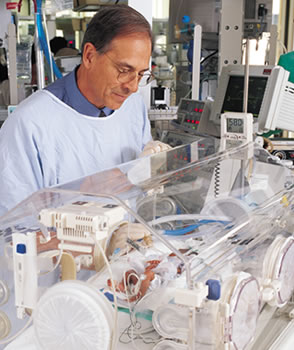
mother’s womb. ![]() A cadre of specialists at the University of Miami School of Medicine,
from seasoned physicians to nurses and respiratory therapists, buzz through
the Neonatal Intensive Care Unit, watching the preemies carefully, documenting
checks and balances, attuned to every soft hiccup and labored exhale.
A cadre of specialists at the University of Miami School of Medicine,
from seasoned physicians to nurses and respiratory therapists, buzz through
the Neonatal Intensive Care Unit, watching the preemies carefully, documenting
checks and balances, attuned to every soft hiccup and labored exhale. ![]() While
medical advances in the past decade have dramatically increased the chances
at life these fragile babies will get, physician-scientists at the School
of Medicine’s Division of Neonatology are pursuing promising new
treatments. Their research projects encompass the latest expertise and
technology aimed at helping these babies, and their worried parents, breathe
a little easier.
While
medical advances in the past decade have dramatically increased the chances
at life these fragile babies will get, physician-scientists at the School
of Medicine’s Division of Neonatology are pursuing promising new
treatments. Their research projects encompass the latest expertise and
technology aimed at helping these babies, and their worried parents, breathe
a little easier. ![]() Although
the human respiratory system begins to develop as early as the fourth
week of gestation, crucial aspects for lung function are among the finishing
touches nature bestows on a baby in final preparation for its introduction
to the outside world. And when a baby makes that introduction even a month
too early, its immature lungs present some of the most common, yet some
of the most dangerous, obstacles to its health and ultimate survival.
Although
the human respiratory system begins to develop as early as the fourth
week of gestation, crucial aspects for lung function are among the finishing
touches nature bestows on a baby in final preparation for its introduction
to the outside world. And when a baby makes that introduction even a month
too early, its immature lungs present some of the most common, yet some
of the most dangerous, obstacles to its health and ultimate survival. ![]() “When
a baby is born prematurely, the lungs are anatomically not fully developed,”
says Eduardo Bancalari, M.D., professor and director of the Division of
Neonatology. “They also are biochemically immature.”
“When
a baby is born prematurely, the lungs are anatomically not fully developed,”
says Eduardo Bancalari, M.D., professor and director of the Division of
Neonatology. “They also are biochemically immature.”
Flared nostrils, rapid breathing, and audible grunting are sure signs that a premature infant is suffering from Respiratory Distress Syndrome, the most common lung disorder prevalent among neonates. The cause is a deficiency of surfactant, a substance essential for proper respiration that begins to be produced in the final weeks of gestation. A baby born too early, therefore, misses this crucial step and suffers the consequences as soon as the first gasps of air touch its fragile lungs. From this lack of oxygen stems distress in other systems of the infant’s body as well.
“Every organ depends on the supply of oxygen to the cells,” Dr. Bancalari says. “So if the baby has severe respiratory failure and is not treated properly, or we are not able to maintain the baby’s oxygenation, then every other organ will suffer.”
The proper treatment to which he refers is the routine administration of synthetic surfactant. Surfactant, short for “surface-active agent,” performs just the function that its name implies. When dry air meets wet lung tissue upon inhalation, surface tension is created. Surfactant is a foamy liquid that the body produces to act against surface tension and prevent the alveoli, millions of air sacs in the lungs, from collapsing under the pressure. In the past decade, synthetic surfactant has become a lifesaver that consistently promotes normal respiration in premature infants.
“There’s a dramatic improvement. As soon as we give the surfactant, the oxygenation improves, the lungs start expanding, and the X ray gets much better. Everything improves within minutes,” Dr. Bancalari notes. “That then allows us to lower the pressures and the oxygen concentrations in the ventilator—to minimize or eliminate lung damage.”
Reducing the damage caused by the mechanical ventilation necessary to maintain respiration in the majority of these babies is the focus of a number of research projects being conducted by Dr. Bancalari and his team of neonatologists. Their work is under way at the School of Medicine’s recently opened Batchelor Children’s Research Institute, a state-of-the-art facility dedicated to investigating pediatric diseases and disorders, as well as finding their cures.

“Mechanical ventilation of a premature baby can cause inflammation in the lungs,” explains Cleide Suguihara, M.D., associate professor of pediatrics and director of the Neonatology Physiology Laboratory. “We are looking at what medications we can use to prevent the inflammatory process that takes place.” The corticosteroids that are routinely administered can have developmental side effects, prodding scientists to search for safer alternatives.
Aside from inflammation in the premature infant’s already weak lungs, pressure from mechanical ventilation can lead to a serious complication called broncho-pulmonary dysplasia (BPD). BPD can result in chronic respiratory problems as the infant continues its development outside the womb and, in some severe cases, can hinder normal respiration for years. UM neonatologists are leading research to challenge these conventional machines that treat, yet still harm, the tiny preemie.
“The ventilator really is a double-edged sword,” says Dr. Bancalari. “It’s necessary, and without the ventilation the babies don’t survive. On the other hand, we are doing something that is completely non-physiologic.”
Although her two sons, now eight and 11 years old, received mechanical ventilation treatment following their preterm births, Maria Castro still was not completely used to the idea when her daughter Cecilia was delivered prematurely last February.
“It’s like you have a sheet in front of you,” she recalls of her reaction to the massive machines keeping her tiny daughter alive. “You are in denial. But it’s amazing what medicine can do.”
From a lack of surfactant and, consequently, immature lung function, Cecilia’s right lung collapsed at birth. A slew of medical complications, including BPD as a result of pressure from the ventilator, followed, but she’s fighting for her young life. Born after only 28 weeks’ gestation and weighing just over two pounds, Cecilia has spent more than half of her first year in intensive care.
In efforts to develop a safer and gentler method of respiration treatment for preemies, Dr. Bancalari and biomedical engineer Nelson Claure of the Department of Pediatrics have digitally manipulated mechanical ventilation. Previous clinical studies have shown that dispensing small volumes of gases at a high frequency reduces lung damage. These findings set the standard for the treatment Dr. Bancalari and Claure sought to administer with an enhanced ventilator. Since most preemies are not suffering from severe respiratory distress and do slightly inhale and exhale on their own, the healthiest ventilation therapy would factor in the optimum volume of gas at the best frequency, relating to the baby’s own effort.
 |
||
 |
“In the last few years, we have been working on the idea that computers can take over the management of the ventilator more efficiently,” Dr. Bancalari explains. Working closely with Claure, the research team has developed algorithms that allow a computer in the ventilator to gauge the infant’s condition second to second and provide oxygen accordingly. Studies also are under way to streamline the ventilation treatment even further, programming the computer to continuously measure the concentration of oxygen administered in relation to each baby’s requirements, which often change at close intervals.
Those needs are largely affected by neurological respiratory control, or lack thereof, in the infant’s brain. Preemies not only have immature lungs, but immature brains as well, and sometimes suddenly stop breathing. This is known as apnea, and Dr. Suguihara is closely studying the amino acid neurotransmitters that control respiration in the neonate. The aim is to identify the causes and culprits of erratic breathing in order to develop medications to treat apnea or prevent it altogether by promoting the baby’s neurological maturation.
In healthy full-term infants, the respiratory system develops a biological mechanism to account for damage to the lung brought on by an excess of oxygen or other such compounds and also to prevent BPD. But, as with a deficiency in surfactant production, the preterm infant’s incomplete respiratory development hasn’t allowed for complete maturation of this network, called the antioxidant enzyme system.
Ilene Sosenko, M.D., professor of pediatrics and associate director of clinical development and outreach, is investigating various hormones to find out if they can be used to boost the development of the antioxidant system.
“Steroid hormones, often given to mothers to try and prevent respiratory distress syndrome by causing the lungs to have accelerated development as far as surfactant, also accelerate the development of the antioxidant system,” Dr. Sosenko says. “So they may have several positive effects on the lung.”
Dr. Sosenko’s next research project is a study of ibuprofen to treat patent ductus arteriosus, a condition in which an important blood vessel that is present while the baby is developing in the uterus does not properly close after premature birth to establish normal lung and cardiovascular function.
“We’ve been using indomethacin, a medication with significant side effects,” she says of the current treatment for the disorder. “It would be important if we could find another medication that would do the same type of thing, but not cause the same types of complications.” Ibuprofen seems ideal and will be a major focus of the study.
Future projects for the Division of Neonatology include research on genetic predisposition to BPD, studying slight sedation to ease the discomfort of ventilation, and recruiting specialized physician-scientists as a means to these ends.
The philanthropic foundation Project: Newborn continues to provide the division with research endowments, funds for clinical necessities, and advocacy support, as it has since the organization’s inception in 1973.
Additionally, with UM/ Jackson’s involvement in the nationwide Neonatal Network, another decade of research and medical advancements may bring an end to chronic respiratory problems in the preemie. The coalition conducts studies on a variety of disorders that threaten the health of preterm infants, including projects on nutrients such as vitamin A and their effects on respiration.
Judging from the progress made in the past decade, along with the dedication and innovation of the School of Medicine’s neonatology research team, the prognosis for continued advancement looks promising. And that has physicians, parents, and their delicate infants, breathing a sigh of relief.
Photography by John Zillioux and Donna Victor.