|
||||||||||||||||
|
Dr. Eisdorfer estimates that only about 20 percent of mental health problems are diagnosed. The Center on Adult Development and Aging, the Center for Research and Education on Aging and Technology Enhancement, and other initiatives at the School of Medicine are exploring depression in the elderly and their caregivers, the use of computers and other technology to enhance well-being and support, and the incidence and prevention of suicide in older people. Spiritual care also has been shown to have tremendous impact. “We’ve known about this in cancer and terminal illness for awhile,” says Dr. Eisdorfer, who is a strong proponent of expanding the universal definition of health care to include mental health. “We’re talking about raising the index of suspicion that part of a patient’s problem is mental health.” The result, he is convinced, would be hefty cost savings and a significant improvement in overall health.
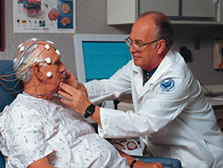
“Seizures in our senior citizens are very frequent and under-recognized,” Dr. Ramsay says. Patients and even many doctors don’t recognize them because they don’t look like the seizures that occur in younger people. “A convulsion is hard to ignore,” Dr. Ramsay says. “The patient falls down, jerks all over, and is usually taken to the emergency room.” But an elderly person having a seizure may just stop what he’s doing and stare into space. “It’s not as overt, but it has some tremendously terrible aftereffects,” he says. The confusion and disorientation may last days, even a week. Coordination is impaired, which often leads to falls and debilitating injuries such as fractures of the hip or leg. “Because these manifestations of seizures haven’t been appreciated, when somebody comes in with a memory disorder, it’s attributed to the aging process or to Alzheimer’s,” he adds. So the right questions are not asked and the patient may not end up with the proper medication to stop or at least reduce the suffering. Dr. Ramsay is involved in a 17-center Veterans Administration study to figure out which seizure medications are best tolerated in the elderly. Other studies have shown that side effects in older patients are two to three times higher than in younger people, at least in part because they take so many other medications. One way researchers found patients for the VA study was by “scrounging through the wards,” Dr. Ramsay says. “Three-fourths of the doctors who saw these patients originally were not thinking epilepsy at all.” Epilepsy results from scarring of the brain, which can be caused by a head injury or stroke in the elderly. Cells on the brain’s surface lose their normal function, resulting in excessive electrical activity that Dr. Ramsay calls “brainstorms.” In many cases an EEG, or electroencephalogram, shows the damage. James Crossman joined the study after suffering a seizure three years ago that was blamed on low sodium. “I was dropping everything,” says Crossman, 65. While he was registering at the VA Medical Center for treatment, he passed out. When doctors determined his sodium was low, Crossman was put on eight medications. After suffering a few more seizures in which he would just go blank, he was referred to Dr. Ramsay. Crossman says he began feeling better when he stopped taking the eight original pills and started one of the study medications.
The study is comparing the anticonvulsant drug carbamazepine, marketed as Tegretol and fairly widely prescribed for seizures in the elderly, with two newer drugs: gabapentin (brand name Neurontin) and lamotrigine (brand name Lamictal). “If we can find a drug they can tolerate, most seizures can be controlled,” Ramsay says. “We’ve had tremendously good results.” A growing and similarly under-recognized problem in older people, particularly in South Florida, is HIV infection. Nationally, 11 percent of people with AIDS are over age 50; in South Florida the percentage climbs to 14. The rate of infection is increasing in older people for two reasons, says Karl Goodkin, M.D., Ph.D., professor of psychiatry and behavioral sciences. The first is that because of the effectiveness of antiretroviral drugs and other therapy, people with the disease are living longer than ever before. The other is that people over age 50 are becoming infected at a higher rate. “Older people have not deemed themselves at-risk and therefore have not been following precautions,” Dr. Goodkin says. “Likewise, doctors have not deemed older people at-risk and have not screened them. They get diagnosed far too late—and at an alarming rate in the month prior to death.” Despite the growing number of older people infected with HIV, relatively little research has been done on the effects of age on HIV symptoms and disease progression. The absence of information concerns Dr. Goodkin and others because the time from HIV infection to the development of full-blown AIDS appears to be much shorter—5.5 years compared to 9.8 years—in older people than in younger patients. Dr. Goodkin is conducting a study, funded by the National Institute of Mental Health with the support of the National Institute on Aging, of cognitive disorders in older HIV patients. Early findings of the study, which will enroll 286 participants, are showing that HIV-positive patients are more prone to have symptoms of minor cognitive-motor disorder: mental slowing, impaired memory, motor slowing, incoordination, irritability, difficulty concentrating, unstable moods, and personality changes. Dr. Goodkin has found differences in immune function in older HIV patients as well. They have been shown to have a lower CD4 cell count—the “helper” cells destroyed by the virus—which means the patient will be more prone to illness due to immunosuppression. There also appears to be a higher CD8 cell count in older people, which probably reflects a higher viral antigenic burden.
“We all have cumulative trauma as we age, but it’s a lot worse with spinal cord injury,” says Dr. Sipski, who is project director for the South Florida Spinal Cord Injury Model System. Last summer the UM/VA affiliation also was designated a Center for Excellence in Functional Recovery in Chronic Spinal Cord Injury, one of 11 VA Rehabilitation Research and Development Centers of Excellence. A wealth of projects is under way to develop treatment for the pain and spasticity of spinal cord injury, to improve bowel and bladder function, to build muscle mass, and to reduce the elevated risk of cardiac disease that comes with such an injury. Those problems naturally have escalated as the life expectancy of injured patients has increased. “People with spinal cord injury age more quickly,” Dr. Sipski says. The problems that develop can be related to overuse or underuse: Arms, for example, are not built to bear as much weight as they must for patients with spinal cord injury. The result can be carpal tunnel syndrome and other musculoskeletal complications. Research is targeting the changes in lipid profiles that develop with spinal cord injury, raising the risk of heart disease. The incidence of diabetes is higher as well, and the skin problems that go along with the injury become repetitive with aging. Some of the problems are secondary effects of the treatment patients receive—for instance, catheters can cause infections. And there is a higher risk of bladder problems, including bladder cancer and renal failure. Other researchers are studying cultural differences in the function of patients with spinal cord injury. “We really have to look at this population in terms of what can be done to help them maintain function as much as possible,” Dr. Sipski says. “We want to keep them out of nursing homes.” |
||||||||||||||||
|
|
||||||||||||||||
|
Christine Morris is executive director of media relations
for the School of Medicine.
Illustration by Polly Becker. Photography by Donna Victor and John Zillioux. |
||||||||||||||||
|
|
||||||||||||||||
|
|
||||||||||||||||