 |
 |
 |
|
 |
|||
 |
|||
Rarback and Benke served
as members of the state’s
Newborn Screening Advisory Task Force, which presented a comprehensive
report and recommendations on expanding the state’s screening program
to the governor and legislators in the fall of 2002. The task force’s
recommendation was to expand the state’s screening to 23 disorders,
funding the expansion through general revenue. That initiative appeared
to have stalled in Tallahassee—until now. The lack of movement
was frustrating to frontline health care providers because they know
the consequences when one of these disorders is missed. And they know
how quickly the window for therapeutic intervention can close.
“We have an interval of less than 10 days of life to get these kids in and prevent them from having irreversible damage,” Elsas says.
The Tale of Two Disorders
![]() tephen Magee is 15 years old, an honors student, and an aspiring rock
star. Nicholas Villanueva is 6 years old, has had half his brain surgically
removed,
and is learning how to drink from a cup. They were both born with metabolic
disorders that can be picked up through a simple blood test at birth. Stephen’s disorder
was discovered—Nicholas’s was not.
tephen Magee is 15 years old, an honors student, and an aspiring rock
star. Nicholas Villanueva is 6 years old, has had half his brain surgically
removed,
and is learning how to drink from a cup. They were both born with metabolic
disorders that can be picked up through a simple blood test at birth. Stephen’s disorder
was discovered—Nicholas’s was not.
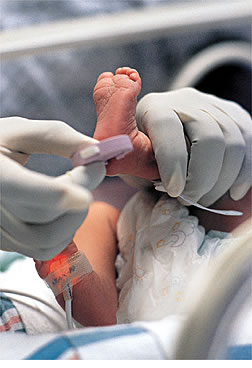
When Stephen Magee was born, his heel was pricked
for a few drops of blood and sent to a lab to be tested. Shortly after
his mother, Norma, brought him
home
from the hospital, she received a phone call from the Mailman Center for
Child Development saying he had tested positive for phenylketonuria,
more commonly
known as PKU. The Central Florida-based mom had never heard of either Mailman
or PKU, so she politely said, “We don’t want anything, thank you
and good-bye.” And she hung up the phone. Stephen’s pediatrician
then called, and Stephen was on his way to Miami for the first of many, many
visits.
 |
||
 |
||
Nicholas Villanueva has been less fortunate. Nicholas was born with VCLAD deficiency, a metabolic disorder that is also detectable by a blood test at birth. But his disorder was not picked up because the State of Florida did not test for fatty acid oxidation disorders like VCLAD. Nicholas, the third of three boys, was a happy, healthy child who was developing normally until he suffered about of flu at 15 months old. Like many people with the flu, he didn't’t want to eat much. Unlike other flu victims, though, that fast would nearly prove fatal.
Nicholas’s lack of food intake caused severe hypoglycemia, which led to a massive stroke. After his stroke, Nicholas “was a vegetable,” says his mother, Irene. Intensive therapy, medication, and feeding through a tube in his stomach helped Nicholas enormously, but he suffered nearly constant seizures. In the summer of 2001, the right half of Nicholas’s brain was removed to alleviate the five to 15 daily seizures.
Today, Irene says 6-year-old Nicholas is “delayed. He understands everything that you say but he just can’t get the words out. He has a left-side deficit and he wears a brace. He does pretty much everything that a kid does, with the exception that he’s probably developmentally between a 2- and a 4-year-old. We just don’t know where he’ll be,” Irene says. The Villanuevas moved to Florida from New Jersey shortly before Nicholas was born. Infant screening programs in New Jersey test for fatty acid oxidation disorders.
Outmoded
Techniques
![]() esides
testing for only five disorders, Florida also has used outmoded techniques
for its testing, increasing the chances that these disorders can be
missed. Take, for example, the number of babies who are diagnosed with
galactosemia in this state. Babies with galactosemia lack an enzyme
needed to break down the milk sugar galactose. If galactosemia is not
detected, babies can suffer brain damage, liver damage, cataracts,
or death. Because milk—either breast milk or formula—is
all a newborn baby is fed, babies can deteriorate rapidly if the disorder
is undetected.
esides
testing for only five disorders, Florida also has used outmoded techniques
for its testing, increasing the chances that these disorders can be
missed. Take, for example, the number of babies who are diagnosed with
galactosemia in this state. Babies with galactosemia lack an enzyme
needed to break down the milk sugar galactose. If galactosemia is not
detected, babies can suffer brain damage, liver damage, cataracts,
or death. Because milk—either breast milk or formula—is
all a newborn baby is fed, babies can deteriorate rapidly if the disorder
is undetected.
But in Florida, “if you count the number they [state officials] say they are detecting, the number of babies diagnosed is at about 50 percent of known gene frequency,” Elsas says. “So the others are just not being identified.”
![]()
Elsas, one of the world’s leading experts on galactosemia, is currently testing a noninvasive breath test that would detect galactosemia before the newborn leaves the hospital. This would supplement the blood test mailed to a centralized lab that yields results in one to two weeks.
 |
||
 |
||
Florida’s newborn screening program is currently supported by a hospital assessment fee for each live birth. Recently, the State of Florida was able to lower the fee hospitals pay and at the same time maximize Medicaid dollars to support the program, which freed up the funds necessary to pay for the program.
But the new expanded screening will require not only new equipment and a diagnostic lab but also the creation and adoption of a multifaceted treatment program to support the increased numbers of infants who will be diagnosed with these diseases. “That’s the other part of it—it’s not just buying a machine, it’s creating a program,” Rarback says.
For example, a nutritionist who specializes in metabolic disorders, like Rarback, spends dozens of hours working with individual patients on diet plans. When more disorders are detected, more specialists will be required to meet the needs of these patients. An entirely new program and process would need to be in place.
“The program would have five parts to it: screening, which is identifying a large number of all newborns and a smaller number who are at risk, but doesn’t identify the disease,” Elsas says. “So you have to have a second process that is immediately available to either confirm the screening [make the diagnosis] or determine that the screening result was a false positive and reassure the parents and physician. If the diagnosis is confirmed, you have to have trained health professionals who know how to take care of those disorders. This fourth component is the intervention itself, the treatment. What do you do with a truly positive baby? Some of these have very complicated disorders and may require level three newborn intensive care units to work with the medical geneticists.”
Finally, in a “truly ‘public health’ program, the public wants to know what has been accomplished, so you have the accountability component. You want to know what the outcome was—when did you identify the child and when did you treat? Did the screening work? What was the immediate effect of the treatment? What was the long-term effect? Those are the databases that should be developed so you could go back to the legislative branch and your elected officials and say we used your tax dollars wisely,” Elsas says.
It is a daunting, but not impossible, mission. “It’s in the public interest to predict and prevent these disorders, and it’s economically as well as emotionally appropriate, because a tax dollar that is put into the program will have a cost-to-benefit ratio that is quite large,” he says. Even though the new screening is expected to net approximately 74 sick babies out of Florida’s annual 200,000 births, the savings could be enormous. Every missed baby, like Nicholas, can cost millions of dollars in care.
It is much more than an economic issue, of course. With these diseases families are devastated and, most tragically, children are disabled. These are the children who come to the Miller School of Medicine after it’s too late to reverse the damage that has been done. They are why Elsas, Rarback, Howell, Benke, and others have spent so much time trying to convince the state to expand its infant screening program.
“This is for Florida’s children,” Elsas
says. “We’re happy that the state has finally come forward
and declared their support for them.”
Robyn Nissim is the editor of Miami Medicine.
![]()