 |
 |
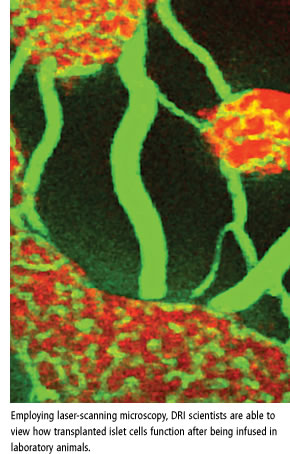 For the first time ever, scientists can view how transplanted insulin-secreting cells called islets function when they are inside a living organism. Researchers from the Diabetes Research Institute (DRI) at the Miller School and Karolinska Institutet in Stockholm, Sweden, published their findings in Nature Medicine. Although still in the experimental stages of clinical research, islet cell transplantation is currently considered the most promising method for curing type 1 diabetes. For the first time ever, scientists can view how transplanted insulin-secreting cells called islets function when they are inside a living organism. Researchers from the Diabetes Research Institute (DRI) at the Miller School and Karolinska Institutet in Stockholm, Sweden, published their findings in Nature Medicine. Although still in the experimental stages of clinical research, islet cell transplantation is currently considered the most promising method for curing type 1 diabetes.
“Up until now we have had no clear way to directly view and monitor how transplanted insulin-producing cells function after they are infused into a patient,” explains Camillo Ricordi, M.D., scientific director of the DRI. “This new technique allows us to study transplanted tissues with sophisticated multiphoton confocal microscopy technology, as if we were observing the transplants through a window in real time. One of the biggest problems with islet cell transplantation has been having enough of the insulin-producing cells survive the transplant process itself; now we have a window into that living world and this will expedite research considerably.”
The DRI scientific team transplanted pancreatic mouse islets into the anterior chamber of a mouse eye and then viewed the transplant through the cornea, as if it were a living window. After transplantation, the islets actually engrafted on the iris, became vascularized and innervated, retained their cellular make-up, responded to stimulation, and actually reverted diabetes in the animal—processes that were able to be watched for the first time as they unfolded.
 “Using novel laser-scanning microscopy allows you to see deeper into tissue,” explains Alejandro Caicedo, Ph.D., research assistant professor of surgery at the DRI and one of the senior authors of the study. “One of the things we were able to see right away was how the islets established their blood supply, which is a crucial step in the transplantation process because islets need a large blood supply to survive. Although islets make up 1 percent of the pancreas, they get as much as 40 percent of the organ’s blood supply.” “Using novel laser-scanning microscopy allows you to see deeper into tissue,” explains Alejandro Caicedo, Ph.D., research assistant professor of surgery at the DRI and one of the senior authors of the study. “One of the things we were able to see right away was how the islets established their blood supply, which is a crucial step in the transplantation process because islets need a large blood supply to survive. Although islets make up 1 percent of the pancreas, they get as much as 40 percent of the organ’s blood supply.”
Using this novel technology, DRI researchers were also able to watch how the immune system launches its attack on the islet cells, something that occurs in the natural course of type 1 diabetes onset. This viewing platform also gives scientists a way to watch the body’s response to new therapeutic strategies that attempt to save islets from this deadly immune system attack. |
 |
 |


