|
 |
Flights of Hope
By Maya Bell
 |
| Twenty hours after the devastating earthquake, the Miller School’s Barth Green, M.D., landed in Haiti with Leo Harris, P.A., and three other trauma specialists to begin saving survivors. |
January 12
Shortly before 5 p.m. that Tuesday, Junior Clermond left his friends on the street and climbed the stairs to his Port-au- Prince apartment. As he reached the living room, the building began to shake violently. Racing down the steps, Junior almost made it outside when the iron entry gate toppled, pinning him underneath. A chunk of concrete smashed his forehead; more debris pelted his back, arms, and legs, trapping him in what he feared would be his tomb.
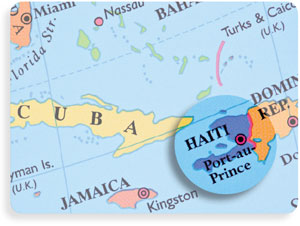 |
| Located in the Caribbean about 750 miles southeast of Florida and just east of Cuba, Haiti occupies the western third of the island of Hispaniola, which it shares with the Dominican Republic. |
“I couldn’t feel anything," the 19-year-old student remembers. "I saw an arm under the gate but I didn’t know it was mine—until I finally recognized my watch."
Seven hundred miles away, Barth Green, M.D., professor and chair of neurological surgery, was finishing his Tuesday spinal surgeries at Jackson Memorial Hospital when a Project Medishare volunteer sent him a frantic text message from New York: A 7.0-magnitude earthquake had devastated Port-au-Prince. Were Medishare volunteers in Haiti OK?
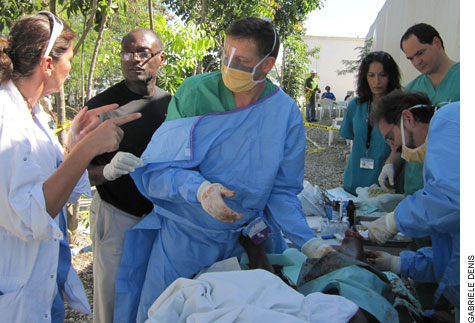 |
| At right, a Martinique doctor confers with Edgar Pierre, M.D., and Daniel Pust, M.D., who is helping Enrique Ginzburg, M.D., amputate a foot outside the U.N. clinic. |
At the time, Green couldn’t fathom that the Western Hemisphere’s deadliest earthquake would leave an estimated 300,000 people dead, more than a million displaced, and tens of thousands with fractured and crushed limbs or other lifethreatening injuries. He had no idea that only two ORs were still functioning in the devastated capital, that an entire class of nursing students had perished in their collapsed school, that three of the nation’s medical colleges lay in ruins.
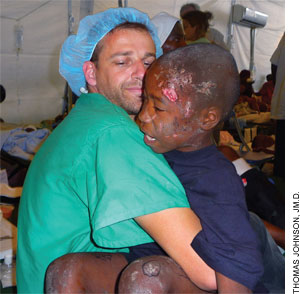 |
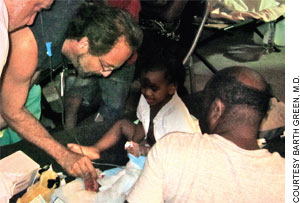
| Pust comforts a 9-year-old orphan injured in the quake. |
But Green didn’t need the details to know Haiti had descended into unimaginable misery. Sixteen years earlier, he and Arthur Fournier, M.D., professor of family medicine and associate dean for community health affairs, had founded Project Medishare to improve the woefully inadequate health care infrastructure in a country still without a single trauma hospital.
So, as Junior’s bewildered neighbors spent the next eight hours clearing away rubble to extract him from his crypt, Green began laying the foundation for the most successful post-disaster rapid-relief response ever mounted by a university, an effort capped by the establishment of the best-staffed, -stocked, and -managed field hospital in Haiti.
January 13
Tapping his vast network of friends, supporters, colleagues, and donors, Green arranged for a friend’s corporate jet to fly him to Haiti the very next morning. He then began making SOS calls to Miller School colleagues at the Ryder Trauma Center, recruiting what would be the first outside medical team to reach Haiti’s devastated capital.
The team—Enrique Ginzburg, M.D., professor of surgery, Edgar Pierre, M.D., assistant professor of anesthesiology and critical care, Daniel Pust, M.D., surgical critical care and trauma fellow, and Leo Harris, a neurotrauma physician’s assistant—brought a breadth of experience from one of the premier trauma centers in the world.
 |
| Ginzburg tends to another boy’s wounds. |
Still, nothing from their extensive training or work history could have prepared them for the carnage they saw when, less than 20 hours after the earthquake, they landed at Toussaint Louverture International Airport with garbage bags stuffed with dressings, saline, IVs, intubation trays, and analgesics. Met by Haitian President Rene Preval and his wife, Elizabeth, the Green team was immediately whisked to a pair of United Nations cargo tents at the airport.
Inside was a scene reminiscent of the Civil War. Nearly 250 people with severed limbs, open fractures, soft-tissue wounds, head trauma, and unknown internal injuries lay on row upon row of cots, screaming and moaning in agony. Blood seeped through dirty bandages and soiled clothes. The stench of urine and rotting flesh, and swarms of flies, choked the air.
Family members of the injured, many gravely wounded themselves, besieged the UM doctors. Exhausted and overwhelmed, Louise Ivers, M.D., who was in Haiti for Partners In Health, broke down in tears. “Thank God you’re here," Ivers, the lone doctor working in the compound, told Green and his colleagues.
“It was like stepping into a horror movie,’’ Green recalls.
“You’re waiting for the director to pop up and yell, ‘Cut!' " Harris added.
“I’ve never seen so much suffering in one place,’’ Ginzburg said. “The immensity was overwhelming.’’
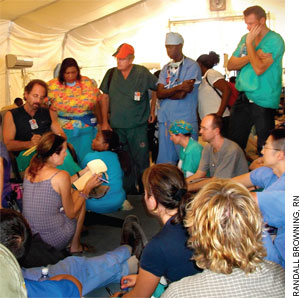 |
| Enrique Ginzburg, M.D., left, leads a discussion with other volunteers about the care of the more than 200 patients in the U.N. tents. |
Shaking off their shock and suppressing their emotions, the UM team quickly set to work. Kneeling at each cot, they inserted IVs for hydration, cleaned and dressed wounds, dispensed painkillers, and set broken limbs with anything they could find—a stick, a table leg, a strip of cardboard. When they reached the last cot, they started anew.
Back on the Miller School campus, the Haiti Relief Task Force, a group of Miller School faculty, staff, and volunteers, began working around the clock to coordinate dozens more flights that, over the months, would transport tons of supplies and most of the 2,700 volunteers from the University and beyond who would staff the makeshift clinic and the field hospital that opened in Haiti just eight days later.
As darkness fell on the clinic the night after the earthquake, Green tasked Harris with accompanying seven of the most critically injured patients to South Florida on the jet that had brought his team down that afternoon. Among them was Christa Brelsford, a graduate student from Arizona State University whose right ankle was partially severed by a collapsing building. In Haiti to help her brother with a literacy project, she would come to embody the indomitable spirit of the many survivors who inspired their caregivers.
“I am so thankful to be alive,” she said, after UM doctors at Jackson Memorial amputated her lower right leg. “And so terribly sorry for the people in Haiti who don’t have adequate medical care.”
Indeed, the UM team would lose their first patients at the U.N. compound Wednesday night: a young man and woman who probably died from blood clots that, under ordinary circumstances, might have been prevented with a dose of heparin. But these were not ordinary times, and doctors accustomed to practicing the best medicine in the world learned to do the best they could with what little they had. They used hoses for tourniquets, concrete slabs for operating tables, colored dots for triaging, heating elements from military Meals Ready to Eat to warm premature babies.
“For 10 days, we had no X-rays, no blood draws, no tests,’’ Pust remembers. “Everything was improvised. We did everything by physical exam.”
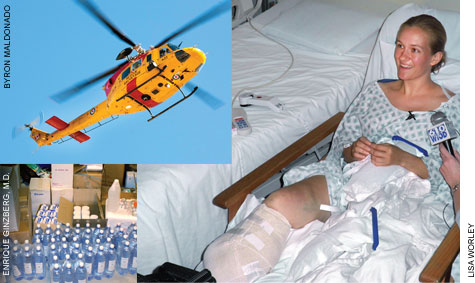 |
| Clockwise from above: Helicopters ferried emergency supplies and personnel, and transported the critically injured. Christa Brelsford was airlifted to the Ryder Trauma Center, where her crushed lower right leg was amputated. Much-needed supplies were stockpiled. |
January 14
On Thursday morning, Ginzburg performed the first of what would be countless amputations outside on a folding table, using only local anesthesia and a scalpel and scissors. The patient was a teenage boy whose family begged the veteran trauma surgeon to remove his fractured arm, already blackened where bone had broken skin. They knew what Ginzburg knew: if the gangrenous infection spread, the boy would die. Instead he became one of the first of Haiti’s estimated 5,000 new amputees.
“It was primitive, but wonderful,’’ Ginzburg said. “We bandaged him and put him in our tent and his whole demeanor changed from sick to calm.’’
January 15
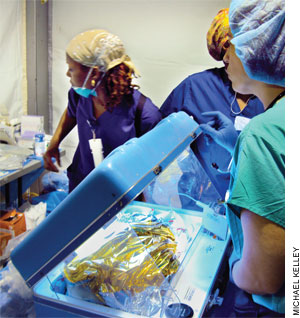 |
| Until these portable light cases arrived, pediatricians used heating elements from military Meals Ready to Eat, or MREs, to warm premature newborns. |
By Friday, reinforcements and supplies began pouring into the U.N. compound from Miami and around the globe, swelling the volunteer staff to more than 100, and enabling exhausted doctors and nurses to work in shifts. But as fast as patients could be discharged, evacuated, or mourned, rescue helicopters, makeshift ambulances, and distraught family members dropped off more. Among them was Junior Clermond, who had been sent home from the local hospital after a doctor stitched his forehead.
Surveying the cramped and unsanitary camp, former Miami Heat basketball star and philanthropist Alonzo Mourning was overwhelmed by the desperation and need. Patients were in agony. Doctors were amputating by flashlight. Volunteers were snatching naps on the ground. And the U.N. needed its tents back. The patients had to go elsewhere.
Mourning asked Ginzburg what he needed. The veteran surgeon didn’t hesitate: “Four large tents,’’ he said, already envisioning the critical care field hospital that the University of Miami would open just six days later on the edge of the airport. Mourning vowed to make it happen.
 |
| Enrique Ginzburg, M.D., Daniel Pust, M.D., and a medic from Portugal load a patient onto a truck for the journey from the U.N. clinic to UM’s field hospital. |
January 16
As Ron Bogue, the Miller School’s assistant vice president for facilities and services, flew to Port-au-Prince Saturday to plan the field hospital, Junior’s condition worsened. He had received liter after liter of IV fluids but was not producing urine. Instead, his legs bloated—evidence that the rapid breakdown of his crushed muscles had released a toxic protein known to trigger acute kidney failure. A common complication of crush injuries, rhabdomyolysis would kill untold numbers of Haiti’s earthquake survivors who, at first glance, seemed to have nothing wrong.
January 17
 |
| From top: A critically injured Junior Clermond is lifted onto a private jet for transport to the Ryder Trauma Center. Months later, Clermond thanks Daniel Pust, M.D., and Antonia Eyssallenne, M.D., Ph.D., before his discharge. |
By Sunday, Junior was in pulmonary failure. Pust and Antonia Eyssallenne, M.D., Ph.D., chief pediatrics resident, knew he would not live another day. Fortunately, Green, who had returned to Miami to coordinate the relief effort, was on his way back to Haiti with Miller School Dean Pascal J. Goldschmidt, M.D. When their plane landed, Goldschmidt and Pust helped carry Junior aboard for the flight back to South Florida. Eyssallenne accompanied the young man, returning to Haiti the next day.
Junior and Christa Brelsford would be among 200 earthquake survivors treated at Jackson, an option that became increasingly unnecessary when, on January 21, the UM Hospital in Haiti (see story, page 12) opened.
...and Beyond
 |
| More volunteers gather at the Port-au-Prince airport. |
In the eight weeks following the earthquake, more than 2,000 volunteers from the Miller School, Jackson Memorial, nearly every state, and several countries treated more than 20,000 patients and performed more than 1,500 surgeries at the hospital. Now in a fixed building, it remains an oasis of hope and a model for the permanent trauma hospital Project Medishare is committed to establishing in Haiti.
As a recovering Junior Clermond said his goodbyes at Jackson, he expressed the deep gratitude of many patients: “Thank you, thank you, thank you,’’ he said. “To God first and then to those who saved my life.’’
Little did he know that all the doctors, nurses, therapists, and other volunteers who rushed to Haiti in its darkest hour were equally grateful for the privilege of serving.
“From day one, it wasn’t about overwhelming challenges; it was all about creating lifesaving solutions,” Green said. “It was a great attitude. But I expected that because they’re all healers.’’
|
 |
 |