 |
 |
Recovering Shattered Lives
By By Maya Bell | Photos by Olga Quintana and John Zillioux
The state-of-the-art technologies and treatments offered at University of Miami/Jackson Memorial Burn Center are complemented by a compassionate commitment to helping patients reclaim their lives while recovering from devastating injury.
 |
| Tommy Gutierrez, then 8, of Hialeah, plays in the pool at Burn Camp with his “burn buddy,” Carl Schulman, M.D., one of the burn center’s three surgeons. |
His face contorted in pain, Devin Olmstead kneels on the mat, bends at the waist, and struggles to balance the weight of his badly burned torso on his outstretched elbows and forearms. “Oww! Oww!’’ the 9-year-old moans, collapsing in sobs. “No more! No more!’’
But occupational therapist Angel Alvarez does not relent. “Come on, Devin, give me five more,’’ he gently coaxes. “Come on, big guy, you can do it.’’
Three days a week, Devin returns to the rehabilitation center at the internationally renowned University of Miami/Jackson Memorial Burn Center for the painful therapy that is rebuilding his strength, improving his range of motion, and stretching the taut, angry-red skin that covers 45 percent of his body and constricts his torso, his arms, his hands, and what’s left of his fingers like a coat of shrink-wrap.
The Pompano Beach fourth-grader has come a long way since that life-altering instant last Memorial Day when the go-cart he’d raced dozens of times flipped and exploded in flames, trapping him underneath and consuming his shirt and skin from chin to belly. After 81 days in the hospital, eight operations, and six weeks in intensive care, Devin is back home with his family, playing video games, annoying—or being annoyed by—his 4-year-old sister, and venturing into the world where strangers often stare. Some even bestow God’s blessings.
The boy’s reply: “Obviously, I’m blessed. I’m here.’’
But Devin, who shuns photographs, still faces a long, difficult road ahead—one that, like thousands of burn survivors before him, he is traveling with members of the burn center’s multidisciplinary team. They are among his biggest fans, his most devoted cheerleaders, and his toughest coaches.

|
| On the helipad where the UM/Jackson Memorial Burn Center surgical team meets critically burned patients: Nicholas Namias, M.D., M.B.A., director and professor of surgery, center, with associate professors of surgery Louis Pizano, M.D., and Carl Schulman, M.D.
|
Consisting of three Miller School surgeons and nurses, social workers, nutritionists, occupational and physical therapists, nurse practitioners, psychologists, and wound technicians from Jackson Memorial, the team sets extremely high goals: They want their patients to regain 100 percent of their functionality and recognize that disfigurement does not define them.
“We never give up,’’ says center director Nicholas Namias, M.D., M.B.A., professor of surgery, pointing to a sign on his office door where a version of the team motto is displayed. “And as much as we can, we don’t let patients give up. We point out they will get better. It will take a long time, but it will happen. Look at Devin. He’s very driven and one day he’ll do almost anything he wants. We all admire that kid.’’
The admiration is a two-way street. Burn survivors who already have made the journey on which Devin is embarking often return to the center to thank the doctors, hug the nurses, and apologize to the therapists for the verbal abuse they often hurled during the long, dark, agonizing months of recovery, rehabilitation, and acceptance.
Now 21, Cooper Grecco has undergone 63 surgeries and procedures since she was badly burned in a car accident at age 16. She remembers loathing Alvarez for waking her every morning to put on socks.
“It hurt so much, but everybody—the doctors, the nurses, the therapists—was amazing. They saved my life,’’ Cooper says. “They not only fixed me physically, but they had a big part in my emotional and psychological recovery. I never thought I’d even walk again, and I’m running and rollerblading.’’
One of the biggest and busiest burn centers in the country, the UM/JM Burn Center is known as much for its advanced burn care, research, prevention, and education programs as it is for its compassion. Of the nation’s 200 designated burn centers, it is one of only 56 and the only one in South Florida to win verification by the American College of Surgeons and the American Burn Association—a true mark of distinction earned in 2008.
|
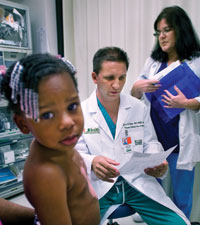
| Louis Pizano, M.D., with an assist from case manager Olga Quintana, M.S.N., A.R.N.P., checks Prosperity Robbins, 2,
of Miami, in the burn center’s outpatient clinic, where burn patients receive long-term wound care and management.
|
Annually, the center’s three surgeons and attending physicians—Namias, Carl Schulman, M.D., M.S.P.H., associate professor of surgery, and Louis Pizano, M.D., associate professor of surgery—treat about 300 admitted patients, half with burns over more than 15 percent of their total body surface. Among the most common causes: smoking in bed, spilling hot roof tar, cooking in hot grease, and plunging into scalding bath or shower water.
Center staffers handle about 2,000 outpatient visits a year, mostly for long-term care of burn wounds, which can take a year to mature. They also help teach 6,000 of Miami-Dade County’s youngest schoolchildren how to avoid burns and fire-related injuries.
About 40,000 Americans are hospitalized for such injuries each year, and about 4,000 of them die—making burns the fifth-leading cause of accidental death in the U.S. But thanks to advances in intensive care treatment, pain management, and wound care, the overwhelming majority—94.4 percent—of patients admitted to a designated burn center survive, according to the American Burn Association.
These survivors include patients who suffer even more extensive burns than Michael Brewer, the 15-year-old Broward County boy who, doused with rubbing alcohol and set afire last year by a gang of vengeful schoolmates, continues his recovery from burns over 65 percent of his body.
Located in the Ryder Trauma Center, the burn center consists of five isolated intensive care beds as well as 20 spillover ICU beds, a specialized hospital ward for non-critical burn survivors, the outpatient clinic for long-term wound care and management, a physical and occupational therapy rehabilitation center, and the largest stockpile of cadaver skin in the state.
Used to temporarily cover open wounds while they heal, cadaver skin is stored in a special minus-80-degree freezer purchased with a grant the center received to prepare for any potential mass casualty after the September 11, 2001 terrorist attacks.
But it is not its cadaver supply, state-of-the-art equipment, advanced burn care and monitoring devices—nor even its verification by two prestigious organizations—that set the center apart. The difference is the team approach to burn care that founding director C. Gillon Ward, M.D., began advancing after joining the Department of Surgery as an associate professor in 1975.
At the time, Jackson’s burn service was comparatively rudimentary. Established after a wooden steamship, the SS Yarmouth Castle, caught fire in 1965 and sank on its way to the Bahamas, it had neither a dedicated burn surgeon nor isolated space to care for the American survivors.
But after several firefighters were injured in an explosion after his arrival, Ward convinced hospital administrators and the public of what he and other burn experts knew: Burn survivors face unique medical, physical, and psychological challenges that require care from a multidisciplinary cadre of skilled professionals.
“Burn treatment truly is a team sport,’’ Namias says. “It’s not like other specialties where the only person who really matters is the surgeon because, afterwards, the care is pretty much the same. Understanding and managing a burn patient’s pain, nutrition, physical and occupational therapy, psychological problems, and wound care is very different from other types of patient care.’’
That’s because burns, especially big burns that consume more than 15 to 25 percent of total body surface skin, trigger a systemic inflammatory response that makes the body go haywire. Without those protective layers of skin, fluids leak, microbes invade, and the body swells, closing air passages. Blood pressure drops and the risk of cardiac arrest and renal, respiratory, and pulmonary failure grow.
Yet patients—and even emergency doctors at community hospitals—are often unaware of the danger.
“A lot of people think, ‘Hey, it’s just skin. Maybe I’ll need a little cream and in a couple of days I’ll be OK,’ ’’ Namias says. “Even when they get here, they think they’ll be able to go to the Keys the next weekend. We have to tell them, ‘Look, this is about to get really, really bad.’ ’’
So bad that many health care professionals avoid burn work. They want nothing to do with the pain-staking recovery process or the daily wound cleaning and dressing changes that are so excruciating for patients.
But most staffers at the burn unit can’t imagine doing anything else and have devoted much of their lives to the center.
|
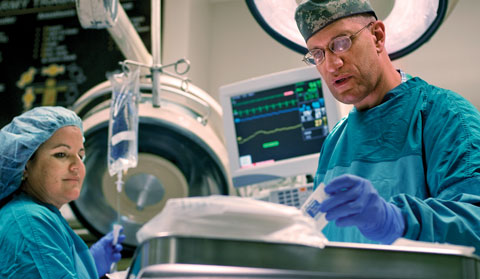
| Burn center director Nicholas Namias, M.D., M.B.A., and case manager Olga Quintana, M.S.N., A.R.N.P., work in a resuscitation room at the Ryder Trauma Center, the first stop for badly burned patients.
|
Clinical nurse specialist Robin Varas, M.S.N., A.R.N.P., and educator Doris Braddy, R.N., B.S.N., joined the unit more than three decades ago. Case manager Olga Quintana, M.S.N., A.R.N.P., started there straight out of college 23 years ago. Alvarez, the occupational therapist, and Sharon Lessner-Eisenberg, the physical therapist, have been there more than 15 years; social worker Leda Borges a dozen.
“Sometimes you wonder if it’s worth it,’’ Varas says. “You’re torturing the patients. But when they come back and say they appreciate the care, they’re glad to be alive, and all the pain was worth it, it’s very rewarding.’’

|
| UM/Jackson Memorial Burn Center occupational therapist Angel Alvarez hugs former patient Cooper Grecco, who has undergone 63 surgeries and procedures since being badly burned at the age of 16.
|
Like Devin and Cooper, most serious burn patients spend weeks under heavy sedation in intensive care, making numerous trips to the operating room so that dead tissue can be excised and open wounds covered, either with grafts harvested from their remaining healthy skin or with cadaver skin. The latter is usually a temporary solution, because cadaver grafts rarely last.
While finding a substitute as good as a patient’s own skin remains one of the holy grails of burn research, UM researchers hope to overcome another obstacle in burn recovery: cachexia, a devastating wasting syndrome characterized by the loss of muscle mass and bone mineral density.
Common in AIDS and cancer patients, cachexia can persist in patients with severe burns for two years, making them susceptible to infection, impeding wound healing, and reducing overall quality of life.
Namias and Teresa Zimmers, Ph.D., a Miller School molecular biologist and research assistant professor of surgery in the Division of Surgical Oncology, believe myostatin, a family of muscle growth regulators, plays a role in the wasting process. With the help of Michael Cheung, M.D., a third-year resident who developed the first model of burn-induced hypermetabolism and muscle wasting, they are exploring the precise impact of myostatin.
Their preliminary data show that inhibiting myostatin at just the right time in the healing phase accelerates the recovery of muscle mass, offering hope that the discovery will lead to the development of a drug that will do the same for burn survivors.
In the meantime, the UM/JM burn specialists are unafraid to pioneer new standards of care—even when it means employing ancient remedies. Amid withering criticism, they were among the first to resurrect the ancient practice of employing maggots to clean wounds.
“Everybody said we were crazy,’’ Namias says. “I remember one of the lions of burn surgery got up at a meeting and thanked me for setting medicine back 200 years.’’
Today many burn centers around the world enlist germ-free, laboratory-grown fly larvae in the battle to clean wounds, and for good reason. As UM/JM specialists proved, maggots are excellent debriders, often outperforming surgeons who invariably take some good tissue when scraping away the bad.
Conversely, fly larvae feast only on dead and infected tissue, killing bacteria, stimulating blood flow, and hastening healing as they release bacteria-killing enzymes.
“I’m really impressed with the way they clean a wound,’’ Varas says. “Sometimes the simplest things are the best.’’
Burn center staffers often say they’d like to put themselves out of business. While that goal is even more elusive than finding a substitute for skin, they have prevented an incalculable number of tragedies through one of the longest-running burn prevention programs in the nation.
Twice a year for the past 23 years, the center and one of Miami-Dade’s seven local fire departments have sponsored the Children’s Fire Safety Festival. Varas and Quintana have helped lead the efforts, which include imparting the dos and don’ts of surviving a fire and avoiding burns to tens of thousands of children in kindergarten through third grade.
Among the lessons delivered through dance, song, and role-playing: Never reach for a pot on the stove. Stop, drop, and roll if your clothes catch fire. Test the water temperature before plunging into a hot bath or shower.
Yet even as the number of children admitted to the burn center declines, the number of senior citizens grows—a byproduct of increased longevity and decreased agility and metal acuity. As a result, Schulman, director of clinical research for the William Lehman Injury Research Center, is using an $80,000 grant to expand the center’s outreach to vulnerable Miami-Dade seniors in their homes.
He and other center staffers also are devoted to helping patients re-enter a world that often doesn’t see beyond their scars. Recruited by Quintana, they volunteer as “burn buddies” at Burn Camp, a four-day getaway at the Elk’s Lodge in Lake County where young burn survivors can forget they look different and have some plain old-fashioned fun.
For Cooper Grecco, nothing has been as liberating or therapeutic. During five trips to Burn Camp—the last one in November—she has watched herself evolve from victim to survivor to role model.
“It’s a weekend of freedom,’’ says Cooper, now a medical assistant in an orthopaedic office. “You’re free to be yourself because everyone has been through the same thing. I wait for Burn Camp all year, and every year I hope I bring more of that liberating feeling home.’’
Devin Olmstead didn’t make camp last November. He was recovering from another surgery to remove scar tissue from his air passage. But the burn team has no doubt he’ll be a role model for other children at camp one day, just as he already is for adults in the rehab center who are just setting out on their own journeys.
Responding to Alvarez’s gentle demand for five more repetitions, Devin dries his tears and begins the painful weight-bearing exercises anew, this time with a whisper: “I think I can do ten.’’
|
 |
 |


